Telehealth physical therapy has gained A LOT of momentum in the past few years. During the pandemic, we saw our profession get serious about remote care. At the same time, we’ve seen patient interest in virtual PT increase as well!
We get tons of questions like:
– “What is telehealth vs. an e-visit?”
– “Is there such a thing as a telehealth physical therapist assistant?”
– “How do I start a telehealth PT business?”
– “What telehealth PT companies are out there and are they hiring?”
– “Does Medicare reimburse for telehealth PT?”
– “How do I center my career around telehealth physical therapy?”

Keep in mind, the field of telehealth is evolving—and so are the answers to these questions. As telehealth establishes itself as a permanent healthcare delivery model, we do our best to keep this article current and reflective of the latest information.
Let’s start with the basics of telehealth PT and go from there!
Table of contents
- What is telehealth physical therapy (PT)?
- How is telehealth physical therapy delivered?
- Why should PTs consider using virtual physical therapy?
- What does the evidence say about telehealth PT?
- Is telehealth PT legal?
- How to become a telehealth PT or PTA
- Telehealth resume for PT, OT, and SLP professionals
- Rules, regulations, and legal considerations of teletherapy
- Telehealth PT CEUs and continuing education
- What does telehealth PT delivery look like?
- What’s it like to be a telehealth PT?
- What does a successful telehealth physical therapist look like?
- What is a typical telehealth physical therapy salary?
- Career paths for the telehealth PT professional
- Telehealth physical therapy in larger systems
- Top resources for teletherapy
- Online physical therapy treatment might play a HUGE role in the future of PT!
This post may contain affiliate links or codes. This won’t increase your cost, but it helps keep TNCPT alive, and free of annoying ads! Thank you for your support. 🙂
What is telehealth physical therapy (PT)?

Simply put, “telehealth physical therapy” (or “virtual physical therapy”) refers to physical therapy services that are provided over a technology platform, rather than in person.
Other phrases referring to telehealth physical therapy might include (depending on your specific role):
telemedicine physical therapy | telePT | teletherapy | telerehab | telemedicine physical therapy | online physical therapy | virtual physical therapy | remote physical therapy | digital PT | digital physical therapy | hybrid physical therapy
How is telehealth physical therapy delivered?
There are four ways to deliver telehealth PT services (source):
- Live video. This is referred to as a “synchronous” format that uses live video interaction between two parties. It’s also sometimes called “real-time.” This type of delivery is ideal for evaluations and treatments.
- Store-and-forward. This is sometimes called an “asynchronous” format. This involves the transfer of health history and/or medical records over secure electronic means. This type of delivery is best for sending x-rays, progress notes, etc. This delivery is scalable, and can also be used for subscription model delivery of services.
- Remote patient monitoring (RPM): This involves the remote monitoring of patients’ health and medical data over secure electronic means. This type of delivery is ideal for monitoring patients’ blood pressure and/or blood glucose measurements, steps per day, etc.
- Mobile health (mHealth): This involves healthcare services, education, and public health notifications being delivered over cellphones, tablets, and other electronic devices. This type of delivery is ideal for alerting patients of updates to their HEP, as well as the closure of roads near a clinic, a possible disease outbreak, etc. Examples of this are WebPT’s HEP software and MedBridge’s HEP program.
Why should PTs consider using virtual physical therapy?
Telehealth PT is now a well-established means to deliver care. While in-person care is (and probably always will be) the norm, there are definite benefits to providing care remotely:
- Emphasizes patient education
- Increases convenience for patients
- Improves access for underserved populations
- Allows for problem-solving in the patient’s usual environment
- Achieves good outcomes
Telehealth physical therapy as a tool for education

While manual therapy is still an important component of our treatments, it’s certainly not the be-all-end-all. In fact, many of us can attest to the fact that too much manual therapy makes our patients dependent upon us, when what they really need is to be up and moving.
As patient education and pain science are increasingly influencing our treatment choices—and ineffective treatment modalities are falling out of favor—we PTs are finding that our role as movement experts relies less and less on patients being physically in the clinic for treatments.
Our primary duty as PTs, aside from doing no harm to our patients, is to educate. Teletherapy is the perfect way to educate patients, promote self-efficacy, and empower patients to take an active role in their healthcare.
Teletherapy as a method of convenience

Now more than ever, we live in an on-demand society. Patients want immediate care, without lengthy wait times or commutes. Plus, people are busy. Fitting yet another in-person appointment into the day just isn’t feasible for some. Rather than forgoing care entirely, telehealth is a convenient way for patients to access care on their schedule.
Telehealth PT as a solution for access
Telehealth is a common-sense solution for what has been called “PT deserts.” That term refers to wide swaths of land where patients have very little access to skilled PT.
The following image, from Omada Health, shows how many PTs there are per 1000 people.
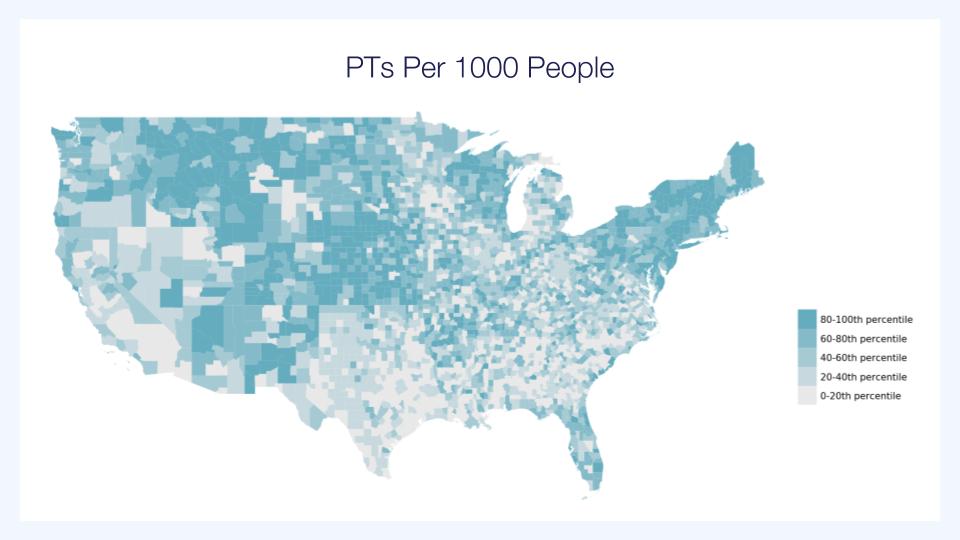
As always, we need to think about how we can best serve our patients. And that means providing them the best possible access to care they might not otherwise get.
Here are a few examples how telehealth PT can help:
- Prevention of readmission through home safety evals and mobility screens
- Post-discharge checkups and safety screens
- Advanced intake of subjective histories
- Wellness and preventative services to avoid hospitalizations
- Consulting with other practitioners (think McKenzie screens, CrossFit/yoga instructors, or pelvic floor consults)
- Post-surgical monitoring and rehabilitation
- Q and A to prevent hospital readmissions and future injuries
Virtual PT as a method for problem-solving
Unlike in-person care, where we can only simulate functional movements, telehealth allows for real-time observation and practice of movements in the patient’s home environment!
This is a great opportunity for collaborative problem-solving, and it has so many applications! From assessing home-office setups to identifying trip hazards, we can make recommendations while receiving real-time input and feedback from our patients.
What does the evidence say about telehealth PT?
What’s popular vs. unpopular doesn’t always matter if the evidence argues otherwise. It turns out that our magical healing hands may only be a small part of the puzzle.
- One 2023 systematic review and meta-analysis found that telerehabilitation demonstrated equivalent or better outcomes in upper extremity motor function, when compared to in-person care for patients with stroke. While the researchers report telerehabilitation can improve therapy adherence after stroke, they found that patient satisfaction levels were “highly variable” across studies. (source)
- Researchers report that telehealth-based exercise interventions are effective for the management of knee osteoarthritis by significantly reducing pain. Telehealth interventions produced similar outcomes compared to controls in physical function and quality of life. (source)
- Seron et al. conclude, “Despite the contradictory results, telerehabilitation in physical therapy could be comparable with in-person rehabilitation or better than no rehabilitation for conditions such as osteoarthritis, low-back pain, hip and knee replacement, and multiple sclerosis and also in the context of cardiac and pulmonary rehabilitation. It is imperative to conduct better quality clinical trials and systematic reviews.” (source)
We’ve seen an uptick in telehealth PT research published in the past few years. That said, much of the recent research we reviewed emphasized the need for higher-quality, well-powered clinical trials to better assess the effectiveness of telerehabilitation. Perhaps you will help add to this growing body of evidence? We definitely need more research physical therapists out there 🙂
Is telehealth PT legal?
YES, telehealth physical therapy is legal. However, every state is different, so you can visit the Center for Connected Health Policy to learn your own state’s rules and regulations, as well as get a better understanding of your state’s parity laws*, if applicable. Plus, standards of practice still hold when you practice telehealth, including:
- Informed consent
- Abiding by HIPAA
- Protecting patient privacy
*Some states have parity laws, which require payers to reimburse for teletherapy at the same rate they would for in-person care. Be sure to know if your state does.
How to become a telehealth PT or PTA
If you’re a licensed PT or PTA, you can practice telehealth. You can join one of the emerging telehealth provider practices as a digital health PT, or you can launch your own telehealth PT practice by using telehealth software and doing your own marketing. Either way, here’s how to get started:
1. Decide whether you want to fly solo or join a company.
This is a big decision based on your own life goals. There are pros and cons to each approach.
2. Get licensed where you intend to practice.
In any case, you’ll need a license to treat your patient(s) where they live. This might sound like a deal-breaker, but a PT compact has been established for this reason. The PT compact is an agreement between member states to enable eligible PTs to work in multiple states under a single agreement.
…If you’re joining an existing practice:
…Explore the telehealth PT companies that are hiring
Here are some companies we know of that offer telehealth physical therapy jobs. We update this list frequently, so you might see it changing as companies shift, change names/practices, etc. If you come across any others, please let us know in the comments below*!
- Agile Virtual PT (virtual PT company that contracts out to work with other clinics, too)
- American Specialty Health (musculoskeletal — PT)
- CityPT (ortho PT)
- eLuma (online therapy for K-12 schools – PT/OT/SLP and some assistants)
- E-Therapy (school-based telehealth – PT/OT/SLP)
- Maven (PT and OT in numerous specialties)
- Omada (adult musculoskeletal – PT)
- Override (chronic pain — PT)
- ProCare Therapy (school-based PT/OT/SLP)
- SWORD Health (adult musculoskeletal – PT)
- Talkpath Live (all ages – PT/OT/SLP and maybe assistants)
- Virtual Physical Therapists (McKenzie certification and/or concussion/vestibular training required – PT)
- WizeCare (PT)
*Please note, there are additional companies like Hinge Health and The Joint Academy, which do hire PTs, but do not necessarily use them to the full extent of licensure.
…Create a telehealth-specific resume and cover letter
You’ll want to really beef up any clinical experience you have, as well as any experience using technology, educating patients, mentoring students, etc. Ensure your resume and cover letter are free from typos, as you’ll be relying on e-communications more than ever as a telehealth PT. You’d better make yourself look good. 🙂
Telehealth resume for PT, OT, and SLP professionals

Telehealth-friendly keywords to include in your resume include:
- Deliver
- Communicate
- Collaborate
- Interpret
- Demonstrate
- Remote
- Educate
- Technology
- Monitor
- Observe
If you’re experienced in Selective Functional Movement Assessment (SFMA), McKenzie Method, or any other functional movement screens or specialized training, definitely highlight that on your resume. Specific ther-ex, vestibular, and/or differential diagnosis con-ed training will also help.
…If you’re starting your own practice:
…Pick a good telehealth PT platform
Some of the following organizations offer software solutions for PTs*:
- Anywhere Healthcare
- BetterPT (soon to be BetterHealthcare)
- BlueJay Health
- BlinkSession
- DrCare247
- doxy.me
- eVisit
- Hello Note
- In Hand Health
- PTEverywhere
- Simple Practice
- TheraNest
- TheraPlatform
- Updox
- VSee
- Zoom for Healthcare
*Please note, there are enterprise-level companies offering telehealth platforms that cater to larger organizations, including Health Recovery Solutions, Force Therapeutics, etc.
…Determine whether you want to be cash-based or collect insurance
Until recently, it was easier to be cash-based, unless you really understood insurance rules and parity laws. However, during the COVID-19 crisis, many third-party payers began to reimburse for teletherapy.
Also, many states have dictated that teletherapy PTs can get reimbursed for telePT delivered to Medicaid patients. You’ll need to check with your specific state for details, though.
Billing nuances to consider for telehealth PT
- Private insurance rules and reimbursement rates vary, and they also vary across state lines. We have linked to resources at the end of the article to help you learn more. Unfortunately, there is currently no comprehensive list of third-party insurances that reimburse for physical therapy telehealth services, and such a list would be nearly impossible to keep current at this time.
- Private insurers often want a written explanation of why telehealth was used. Always keep a record of the services you perform and your rationale for using telehealth vs. in-person visits.
- Currently, there are no CPT codes specific to billing for telehealth physical therapy. Many CPT codes require direct one-on-one patient contact, so telehealth services may not be covered unless there is an agreement with the payer. However, again, check with your insurance partners to know how things are being handled.
Policies are always changing, so check the list of resources at the end of the article for latest info! - Understand billing terminology and nuances. An addendum is often required to be added to the CPT code to denote the service was provided through telehealth. Be sure to check your own insurers’ guidelines.
>>> Use correct terminology for sites.
The originating site is where the patient is located.
The distance site is where you are located.
>>> Use Place of Service (POS) codes appropriately
“02” for telehealth provided other than in patient’s home (patient is not in their home when they receive telehealth services)
“10” for telehealth provided in patient’s home (patient is located in their home when receiving telehealth services)
Please note, telehealth POS codes have been updated in recent years. See Medicare’s list of POS codes for full explanations, and always check with individual payers for their requirements!
>>> Use modifiers properly.
95 = services were delivered synchronously (or in real time for telephone visits, but not e-visits)
GQ = services were delivered asynchronously (this is mostly a form of telehealth getting phased out)
The above codes are subject to change, so please verify with individual payers for latest info and their specific requirements!
Does Medicare reimburse for telehealth PT?
As you might know, Medicare announced that PT, OT, and SLP were temporarily covered services during the COVID-19 public health emergency (PHE). Now that the PHE has ended, the long-term fate of telehealth as a Medicare-covered service is less clear**.
In order to keep our telehealth privileges with Medicare, PTs need to be added to the list of permanent telehealth providers by CMS. This can only happen through the passage of new legislation. For now, you can advocate for new telehealth legislation and keep an eye out for updates from Medicare.
We expect things to change, so please check the resources section at the end of this article for the latest info!
**The proposed 2024 Physician Fee Schedule (released in July 2023) says that Medicare proposes to continue covering telehealth through 2024. Keep in mind that this is only a proposal, so it will need to be passed by the end of 2023 to go into effect. (source)
…Develop a viable business plan
We always recommend any business owner think long-term. Here are some tips to get you started:
- Niche down. Pursuing a niche seems to be the best initial strategy. A niche allows you to create a very specific type of patient base that you can target with your marketing efforts. This works much better than tossing lots of money at marketing to a broad swath of patients, and hoping that you run across a few who decide to take a chance.
Patient niches include: dancers, runners, cyclists, skaters, gymnasts, young moms, patients with chronic CVA impairments, etc. Speciality niches include: ortho, neuro, injury-specific, etc. - Nail down your patient acquisition strategy. Will you be building a therapy website or blog to attract patients? Will you be marketing via YouTube videos?
- Determine your UVP. Your unique value proposition (UVP) will set you apart from the competition. Determine what makes you special and worth working with. Extensive education? Friendly, discreet care? Convenient access?
…Consult with a telehealth PT compliance professional
Because of the nuances involved with transitioning to telehealth, it is always a good idea to consult with a telehealth physical therapy expert—notably, one who understands legal and internet technology (IT) considerations.
Nancy Beckley, MBA, CHC recommends a platform that is HIPAA compliant—with evidence that the platform has complied with HIPAA Privacy, Security and Breach Notification Rules—and a set process for offering a Business Associate Agreement (BAA) as appropriate.
Rules, regulations, and legal considerations of teletherapy
While we’ve covered quite a few of the rules and regulations above, it’s always good to have an attorney weigh in!
We were able to speak about teletherapy with attorney Erin Jackson, Managing Partner of Jackson LLP Healthcare Lawyers. She is extremely passionate about providing this alternative practice setting for PTs, and was eager to weigh in. Here are her thoughts:
- Insurance companies may have requirements—distinct from legal requirements—concerning the frequency, duration, and type of visits that can be conducted via telehealth.
- It’s crucial that providers using telehealth have an up-to-date HIPAA privacy policies and procedures manual. The greater a provider’s reliance on technology, the greater the risk of breach.
- Some states have legislation or regulations which speak to telehealth issues. (This is likely changing on a state-by-state basis.)
- Always check your state legislation regarding direct access considerations.
- Many states have an in-person visit requirement for telehealth-based provider-patient relationships, meaning that it may not be possible to operate a fully telehealth-based practice.
- A PT is still held to the same scope of practice and duty of care. If you can’t offer the same caliber of treatment, the same attention to detail, and the same assessments of functionality as you offer to in-office patients, then telehealth isn’t appropriate for that patient.
The laws surrounding telehealth often lag behind technology, patient demands, and provider capabilities.That’s why it’s essential to stay on top of legal compliance.
Telehealth PT CEUs and continuing education

Technically, you don’t need any additional education to become a telehealth PT. That said, certain skills will make you a much more effective remote therapist.
Examples of helpful training include:
- McKenzie Certification
- Pain science education
- Total Motion Release (TMR)
- Selective Functional Movement Assessment (SFMA)
Telehealth companies look for therapists who can demonstrate a commitment to evidence-based care. Basic educational strategies and treatment with exercise prescription can help many patients feel better.
Telehealth PT CEUs on MedBridge and PhysicalTherapy.com
Many organizations are releasing continuing education courses for PTs, which is nice because you can learn the ropes of telehealth and earn CEUs at the same time. Two of our favorite providers are MedBridge and PhysicalTherapy.com (owned by Continued), due to their ease of use and affordability. By using our discount codes for these platforms, you save money and help support the free content at TNCPT. Thank you for your support!
We’re so excited to share that MedBridge Education now offers a Telehealth certificate program! So, if you’re interested in earning CEUs while you work toward an actual certification to put on your resume, check out this program!

Below, find some excellent individual courses, some of which are included in the aforementioned cert program.
- Telehealth: An Introduction to Virtual Care (MedBridge)
- Starting Out in Telepractice (MedBridge)
- Specialty Work With Telepractice (MedBridge)
- Virtual Pediatric Therapy: Assessment and Intervention Using Telehealth as a Service Delivery Model (MedBridge)
- Telehealth (Digital Practice) Implementation: Considerations and Road Map (PhysicalTherapy.com – use code NCPTBonus13 for a free month)
- How to Make Your Patient Care Virtually the Best! (PhysicalTherapy.com)
- TeleRehabilitation: Demystifying the Use of Technology to Deliver Physical Therapy (PhysicalTherapy.com)

What does telehealth PT delivery look like?

The evaluation
- Past medical history (PMH) + subjective
- Screen for red flags and note tests that require in-person attention
- Functional movement screen + objective measures (modified)
The treatment
- Patient education
- Therapeutic exercise
- In-office treatments as indicated
What’s it like to be a telehealth PT?
Many of you are probably wondering whether you’ll even enjoy being a telehealth provider. It’s wise to consider the pros and cons when weighing this decision.
Pros
- Flexibility. Can you imagine how nice it’d be to treat patients from anywhere that has an internet connection?! Of course, you always want to maintain a safe, private, and secure connection, as well as a professional setup.
- Predictable hours. Generally speaking, you can still have predictable hours when you know you’ll be working vs. not working.
- Using your degree. One of the hardest parts of leaving direct patient care is feeling like you’re not really using your degree. As a telehealth PT, you’re using your degree to its fullest!
- Work from home. Working remotely is fantastic for some people!
Cons
- Difficult patient acquisition. As mentioned above, getting patients is the hardest part. Just like some PTs are disinterested in teletherapy because they don’t understand it, plenty of patients may shy away from telehealth PT because they don’t understand it, or don’t even know it exists as an option.
- Lots of sitting. The nice part is that you’re also up and about to demonstrate exercises, so you’re not quite as sedentary as you might be at other non-clinical jobs.
- Confusing and frequently changing rules and reimbursements. This can be very challenging for those of us who aren’t into following detailed rules and regulations.
- Uncertainty. It’s a newer form of therapy, which can be considered a pro, since there is a lot of opportunity! It’s also hard to find full-time, benefitted roles in teletherapy…at least so far.
What does a successful telehealth physical therapist look like?

- Enjoys patient education. You don’t have those magic hands as your secret weapon to get patients better, so you’ll be relying on your communication and education skills.
- Does not rely on manual therapy alone. For this reason, having sound evaluation and assessment skills, as well as strong patient-education skills, will help you succeed at telehealth.
- Is articulate. When you deliver care remotely, it’s essential to be clear with communications.
- Is tech savvy. When technical issues arise, you’ll need to troubleshoot those yourself—and guide your patients through issues as they happen.
- Is licensed in the state(s) in which they plan to provide therapy. PTs and PTAs can treat as they normally do per a state practice act (with PTAs treating with oversight by a PT). The same goes for OTs and COTAs and SLPs. But if you’re planning to treat a patient in Missouri, you need to have a clinical license (PT, PTA, OT, COTA, SLP, etc.) to practice in Missouri.
- Enjoys patient care. While telehealth PT is incredibly flexible and rewarding, it’s still patient care. It’s not fully non-clinical; it can be considered more of an alternative career for physical therapists. You’ll be providing physical therapy services remotely, so if you truly do not enjoy patient care, you might want to consider something else.
- Has a niche. Whether it’s running, pediatrics, cardiopulmonary, yoga, CrossFit, vestibular, or cycling, patients will be more likely to use your services if you’re considered an expert in your niche.
What is a typical telehealth physical therapy salary?

Most teletherapists do not get a salary, but are paid an hourly wage. That’s because most remote care is delivered on a PRN basis. However, now that many clinics are incorporating telehealth into their existing practice models, this could change. If that’s the case, you can likely expect pay to align with what a staff therapist would make. Experienced PRN telehealth physical therapists typically can earn about $50-75/hour.
Career paths for the telehealth PT professional
Because telehealth PT is a new career niche, only time will tell us what common career paths will be.
Here are just a few that we’re seeing:
- Telehealth PT/A → lead telehealth PT → virtual rehab manager (which likely includes a customer success angle)
- Telehealth PT/A with niche focus → solo telehealth PT with niche independent practice → telehealth clinic manager
- Telehealth PT/A → telehealth consultant→ program manager
- Telehealth PT/A → clinical trainer → training manager
Another thought is to parlay that tech experience into entrepreneurial endeavors, or work for a digital health company as a clinical trainer or implementation specialist.
Telehealth physical therapy in larger systems

Devra Sheldon, PT, MSPT, NCS works at Schwab Rehabilitation Hospital (part of Sinai Health System) in Chicago, which serves many low-income patients who have a tough time getting to appointments. Sheldon has done extensive research into telehealth as a tool for better management of low income populations who have numerous barriers to care, but these barriers can often include lack of the smartphones and tablets used to deliver the very care we wish to provide. So far, this has precluded telehealth from being integrated into their delivery model.
Sheldon is hopeful that hospitals will eventually negotiate with payers and get the ball rolling on insurance reimbursing telehealth for therapy. As an employee of a low-income hospital, she spends a lot of time on the phone and emailing with patients. This time is not reimbursed, even though it’s valuable care. “I believe Telehealth could be very valuable with not just low-income patients, but all patients with persistent pain by evaluating flare ups, reviewing self management strategies, pacing and more,” she explains.
Top resources for teletherapy
Want more information about telehealth physical therapy? Here are some great resources for continued learning!
- APTA’s Telehealth Page – The best resource for telehealth information from the APTA.
- APTA’s Telehealth PT Directory – Add yourself to the list if you’d like!
- AOTA’s Telehealth Resources – The best place to acquaint yourself with AOTA resources regarding telehealth.
- Center for Connected Health Policy – This is where you can look up telehealth rules state-by-state.
- FSBPT – Federation of State Boards of Physical Therapy: resource for state rules/regs around telehealth.
- OT Potential’s Article on Telehealth Occupational Therapy – Great resource for OTs interested in telehealth.
- PT Compact – See which states are members (or in the process of becoming members) of the compact.
- SWORD Health’s webinars. These cover about combining telePT with AI (artificial intelligence)
- WebPT’s free downloadable guide to practicing telehealth – Must sign up for their email list to access.
Online physical therapy treatment might play a HUGE role in the future of PT!
One thing is for sure: telehealth now has a strong foothold as an effective care delivery model.
Whether it’s our main delivery model or an ancillary option to our current models, there is no doubt that, to some extent, online PT treatments are here to stay!
We are eager to hear from you if you have received this type of treatment and/or if you have delivered telehealth. Please comment and let us all know about your experiences!





